Poor ovarian reserve and IVF
Women who plan to get pregnant or have faced some difficulties with fertility usually refer to reproductive clinics to ask for advice on their fertility potential and recommendations for fertility treatments. Many women over 30-40 are diagnosed with something called “diminished ovarian reserve”, and they may mistakenly believe that it is a synonym to infertility. But it isn’t. What does this diagnosis mean? How does it impact the IVF success rate? Is it even possible to have IVF with low ovarian reserve?
Diminished ovarian reserve: what is it and what causes it
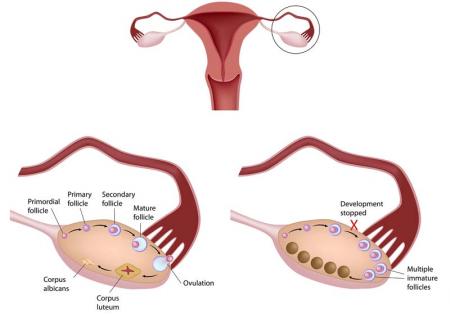
The low quantity of eggs in ovaries is called diminished ovarian reserve (DOR). The reduced ovaries’ egg supply is also associated with the changes in their quality, i.e. their viability, and in how well the ovaries will respond to the stimulation, performed as a part of ARTs such as IVF. In most of the cases, the causes of DOR in women are unknown but they are linked to some health issues such as genetic abnormalities, hormonal disorders, endometriosis, thyroid disorders, exposure to chemotherapy, and pelvic irradiations, as well as some lifestyle behaviours, like stress, smoking, and unhealthy nutrition, etc.
Ovarian reserves diminish over time in all women, the extent to which they do in each woman is unique. But most of the scientists agree that a steep decline in fertility starts in 13 years before menopause. Even though this pattern is pretty clear, two women of the same age may have completely different ovarian reserves and chances of getting pregnant. The problem researchers face in this aspect is that the biological ageing of the ovaries can occur independently of chronological age, so even young women may face the depletion of ovaries’ reserve.
Despite all that, the poor ovarian reserve doesn’t necessarily mean the inability to conceive, it means that the chances are reduced, and it is necessary to improve them with some treatment or lifestyle changes.
Unfortunately, it’s impossible to establish the number of eggs in ovaries accurately; all the existing technologies give rather approximate information. However, several tests nowadays offer the possibility to estimate the remaining pool of viable eggs, including antral follicle count (AFC), Müllerian hormone (AMH), follicle-stimulating hormone (FSH), and clomiphene citrate challenge test (CCCT). The question about which of them works better for diagnostics is still controversial, but it is clear that the woman’s age affects the quality and quantity of her eggs. Some clinics recommend to take at least two different tests to obtain more accurate and exhaustive information and find out how many viable eggs still remain.
Why would a woman want to test her ovarian reserve?
The reasons include the following:
- to predict how many years of fertility she has left;
- to determine her fertility status at this very point of time;
- to predict how well her body will respond to ovarian stimulation prior to IVF.
Low ovarian reserve and IVF success rates

One of the key elements of an IVF cycle is the retrieval of eggs from a woman after the ovarian stimulation. Since DOR is associated with the decline in response to such type of stimulation, and for this reason, the number of eggs ready for collection may be low. If the number of eggs that may be collected is over 10, the prospects for the IVF are really good, if the number is lower than 5, the procedure may be problematic.
The number of eggs that may be retrieved is crucial because, in the IVF procedure, the doctor selects the best eggs for fertilization, and the obtained embryos are tested for deviations. The fewer embryos may be obtained, the higher are the chances that they may present some disorders or chromosomal abnormalities.
Implantation issues are also pretty common among the women who were diagnosed with low ovarian reserves. Such patients may also face some problems with bearing the child, for example, an increased risk of miscarriage after the IVF procedure with their own eggs.
Poor ovarian reserve treatment
The bad news is that there is no treatment for low ovarian reserve because it is a part of a natural ageing process. But there are some options you may use to solve this issue.
DHEA
The ovarian reserve does not rely only on the age of the eggs themselves, another important factor is the quality of the ovarian environment in which those eggs mature. The physician-prescribed dehydroepian-drosterone (DHEA) is used to improve that environment. DHEA is a powerful hormonal supplement that increases androgen levels in women with diminished ovarian reserve.
Usually after undergoing such treatment and improving the ovarian environment, both the quantity and quality of woman’s eggs improves dramatically. This technology sufficiently increases the chances of pregnancy even for the women who are close to the depletion of their ovaries.
Donor eggs
The use of donor oocytes for IVF is another option for women to overcome their fertility difficulties. Reproductive clinics ensure the quality of eggs collected from a donor, fertilize them through IVF, select the best healthy embryos and implant them to the patient’s uterus or surrogate mother’s uterus. This procedure shows higher birth rates than the IVF using the eggs of a woman with low ovarian reserves. Doctors usually recommend this procedure after several IVF cycles fail.
You should understand that even if you are diagnosed with “diminished ovarian reserve”, it doesn’t necessarily mean that you are unable to get pregnant. This condition doesn’t imply that you are infertile; however, it does mean that you may face some difficulties with conceiving. Every case of this condition is unique and the treatment plan should be based on test and examination results.
If you want to find out more about your ovarian reserve or if you are diagnosed with poor ovarian reserve, you may schedule a consultation with a fertility expert to get the help and support you need. By using professional doctor’s advice, you ensure that the obtained information about low ovarian reserve and IVF procedure and treatment services are of the highest possible quality and of reasonable price.

Surrogacy in Ukraine, legal aspects
Infertility treatment by using the services of a surrogate mother is now widely applied in countries where surrogacy...
Should I freeze my eggs
Egg freezing is the set of medical procedures aimed at the preservation of a woman`s fertility. It has already...

What Is Preimplantation Genetic Diagnosis (PGD)
Modern reproductive technologies have evolved and progressed for the last decades which has given a chance for...

What are Surrogacy Contracts
Surrogacy programs require different documents to be signed. This is done to make all the procedures legal and...

What is Gestational Surrogacy and How it Works
Gestational type of surrogacy is considered to be a relatively new method to treat infertility. The 1st baby was...

How Can I Become a Surrogate Mother
The number of couples who start looking at their surrogacy opportunities in Ukraine increases with every year due...

The Egg Donor Process: What to Expect
Becoming an egg donor is both a thrilling experience and big responsibility for many women. It’s a great...

How To Evaluate a Surrogacy Agency’s Success
The surrogacy process is a challenging and exciting journey for intended parents. This procedure requires a lot...

10 Common Questions About Egg Donation
The process of egg donation raises a lot of questions both from recipients and from donors. This procedure is intended...

Fertility after a miscarriage
Fertility is the ability of the female or male body to conceive and give birth to a child. Woman’s fertility...

Difference between primary and secondary infertility
It is only possible to diagnose infertility or sterility, in the case when at the beneficial circumstances, regular...

Signs of preterm labor
Preterm labor poses a threat to the baby’s life and health; though, it could be prevented, if you know about...

Secondary infertility
Infertility is the disorder of the reproductive system, when for a year or more, the attempts to get pregnant are...

Effect of smoking on fertility
Smoking is one of the most widespread bad habits. We have been told about the harmful effect of nicotine starting...

Intrauterine insemination
Artificial insemination is nothing unusual in the modern world. It has been developing the most active in the last...

Alcohol and fertility
Alcohol addiction is one of the most common problems in the modern world. This problem becomes more and more widespread...

Relationship between stress and infertility
From year to year, scientists find more proves confirming the interconnection between stress, depression-related...

Celebrities who resorted to surrogacy
Surrogacy is one of the assisted reproductive technologies. The surrogate mother carries the baby that isn’t...

Endometriosis and IVF
Women who refer to a gynecologist because they can’t get conceive for a long time or who want to try IVF...
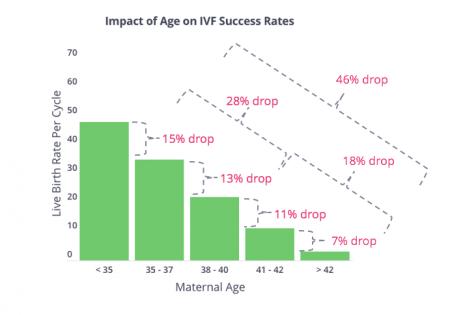
IVF success rates
In vitro fertilization (IVF) is the most efficient and commonly applied type of ART. It is undoubtedly the most...
PCOS and IVF
There are many reasons why woman’s eggs may be of poor quality or quantity. Most common causes are associated...
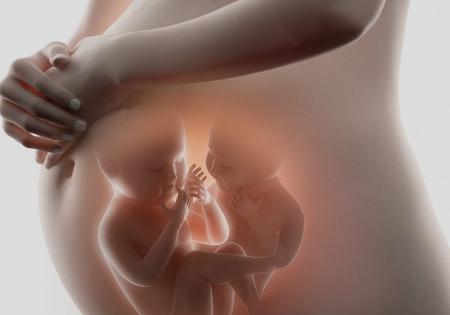
Pregnancy with multiples
Couples planning their parenthood with fertility clinic assistance often inquire about how high their chances are...

What is fertility calculator?
The advance of modern technologies presents a number of opportunities for women to take charge of their fertility....

Male infertility symptoms
The modern pace of life is extremely fast and stressful. We need to keep up with so many things and follow such...

Differences between fresh and vitrified eggs
Many patients who resort for assisted reproduction technologies, like IVF, surrogacy or PGD are often baffled with...

Does age matter for fertility?
How does our age affect our fertility? Age is a crucial factor affecting male and female fertility. The modern...

Egg donation in Ukraine
Egg donation in Ukraine is a trending reproductive service that is becoming more and more popular. For some patients...

Motherhood after 40
The modern world provides women with so many great opportunities but at the same time, it may cause a lot of disappointments....

Why do people choose pregnancy in Ukraine
The modern world presents us with so many great opportunities, the development of the state-of-art technologies...
0817144241_s.jpg)
What is medical tourism?
The globalization of the modern world presents us with a wide range of opportunities for work, recreation,...

Foods that increase fertility
The modern pace of life is extremely demanding: we need to work much, achieve much, and we have no right to fall...

Egg freezing
Egg freezing, also known as the oocyte preservation is a method of woman’s fertility preservation that allows...

How to choose the perfect donor for you
Here are some tips how to choose the perfect donor for you: It goes without saying that your potential...

Agency’s clients need a professional legal support
Anastasia Herman law office provides the full range of effective assistance within Surrogacy, Family and Fertility...

TOP 3 common myths about pregnancy
The mother’s beauty According to a myth, girls steal away their mothers’ beauty. Of course, the truth...

Getting ready for your first visit to a fertility clinic
Take some time to think over and prepare the following information before your visit: List any medications,...
_s.png)
Konsultacja specjalisty z niepłodności Kraków
Jak od dawna starasz się zostać rodzicem, ale tak i nie uzyskałeś dwie upragnione kreski na teście? Ilu lekarzy...
Contact US
Complete the form below to start your journey right now

